- Search
| Ann Coloproctol > Volume 40(1); 2024 > Article |
|
Abstract
Sarcopenia, which is characterized by progressive and generalized loss of skeletal muscle mass and strength, has been well described to be associated with numerous poor postoperative outcomes, such as increased perioperative mortality, postoperative sepsis, prolonged length of stay, increased cost of care, decreased functional outcome, and poorer oncological outcomes in cancer surgery. Multimodal prehabilitation, as a concept that involves boosting and optimizing the preoperative condition of a patient prior to the upcoming stressors of a surgical procedure, has the purported benefits of reversing the effects of sarcopenia, shortening hospitalization, improving the rate of return to bowel activity, reducing the costs of hospitalization, and improving quality of life. This review aims to present the current literature surrounding the concept of sarcopenia, its implications pertaining to colorectal cancer and surgery, a summary of studied multimodal prehabilitation interventions, and potential future advances in the management of sarcopenia.
Sarcopenia is a progressive and generalized disorder of muscle atrophy that is primarily associated with aging, but has also been observed in even younger populations (as early as 30 years) secondary to nutritional deficits, physical immobility, and systemic disease, such as malignancy. Evidence has demonstrated the global prevalence of sarcopenia to be between 10% and 27% in individuals aged ≥60 years [1]. With advances in medicine and overall life expectancy, sarcopenia has been emerging as a significant modifiable risk factor for adverse outcomes in surgical candidates. Specific to colorectal surgery, sarcopenia has implications for early and long-term postoperative outcomes, functional outcomes, and oncological outcomes.
Despite the introduction of Enhanced Recovery After Surgery (ERAS) protocols nearly 2 decades ago, the safety and efficacy of which in colorectal surgery have been observed in large multinational multicenter trials and meta-analyses, complications after colorectal surgery can occur in as many as 45% of patients. Multimodal prehabilitation, as a complement to the perioperative measures of ERAS protocols, offers a potential treatment modality to help circumvent the negative effects of sarcopenia, prepare the patient for surgical stress, and promote earlier recovery [2].
This review aims to present the current understanding of sarcopenia, the effects of sarcopenia on colorectal surgery, potential prehabilitation interventions, and potential future advances in the management of sarcopenia in patients undergoing colorectal surgery.
In the last decade, the International Working Group on Sarcopenia (IWGS) [3], Foundation for the National Institutes of Health (FNIH) [4], Asian Working Group for Sarcopenia (AWGS) [5], and European Working Group on Sarcopenia in Older People (EWGSOP) [6] have established international standards on sarcopenia. The consensus definition of sarcopenia comprises 3 parameters: (1) loss of skeletal muscle mass along with (2) loss of muscle strength and/or (3) reduced physical performance. The presence of all 3 parameters is consistent with severe sarcopenia.
To date, no single diagnostic criterion for sarcopenia has been established, mostly due to the heterogeneity of this disease. Instead, attempts have instead centered on delineating tailored population-based cutoffs. According to the AWGS 2019 update [5], sarcopenia in Asian men is defined as muscle mass <7.0 kg/m2 with a handgrip strength <28.0 kg and/or a gait speed <1.0 m/sec. In women, it is defined as muscle mass <5.4 kg/m2 via dual-energy x-ray absorptiometry (DXA) or <5.7 kg/m2 via bioelectrical impedance analysis (BIA), with a handgrip strength <18.0 kg and/or gait speed <1.0 m/sec.
DXA has high reproducibility but is time-consuming and therefore mainly used in research. In contrast, BIA is quick and inexpensive with reasonable reproducibility and can be used easily for screening. Clinically, because most surgical patients undergo preoperative computed tomography (CT) imaging for diagnosis and operative planning, observational studies have primarily utilized CT scans to define sarcopenia based on low muscle mass. This has been shown to be a useful imaging biomarker for predicting preoperative nutritional risk in elderly colorectal cancer patients [7]. The skeletal muscle index at the level of L3 is the most common measure; however, other parameters, including the psoas muscle area at L4 and dorsal muscle group area at T12, have also been used to diagnose sarcopenia [8]. Muscle mass dimensions on ultrasonography [9] and magnetic resonance imaging [10] are also similarly reproducible and reliable, representing alternative modalities to CT imaging.
Sarcopenia is prevalent in 10% of general elderly patients worldwide [11], in 14.7% of hospitalized older patients [12], 41% to 59% of nursing home residents [13], and 38.6% of cancer patients [14]. While the tumor subsite is one of the major determinants of malnutrition, with pancreatic, esophageal, head and neck, and lung cancer having the highest prevalence [15], sarcopenia is seen in up to 60% of patients with colorectal cancer [16].
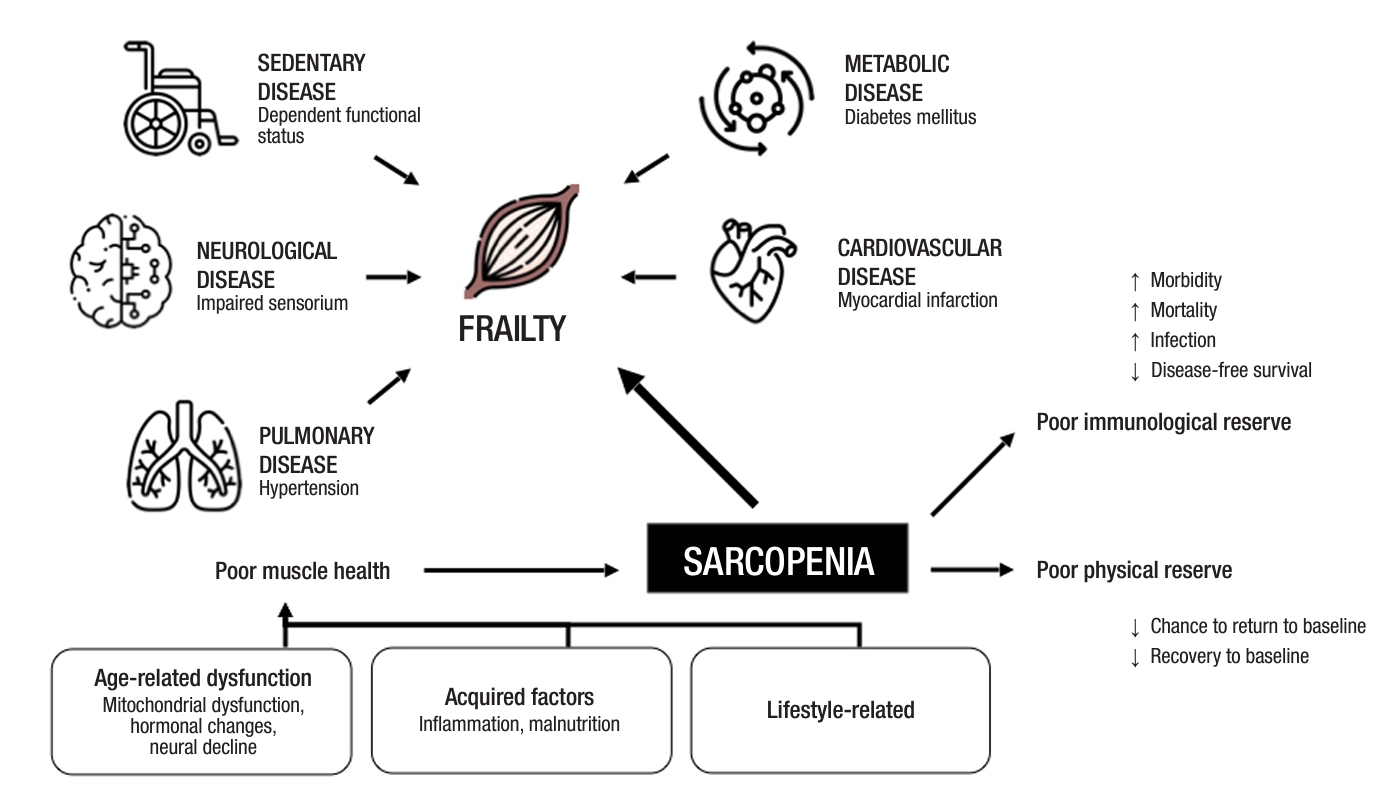
Multiple metabolic processes contribute to the development of sarcopenia over time (Fig. 1). Intrinsic, or nonmodifiable factors include age-related mitochondrial dysfunction and the waning of muscle stem cells’ ability to regenerate. Aging is associated with reduced anabolic efficiency in older adults when compared to their younger counterparts in response to amino acid and glucose-rich food [17], which results in less protein synthesis despite similar diets. This may be mitigated with amino acid or protein supplementation to stimulate protein anabolism, as well as physical activity, which sensitizes aging muscle to subsequent nutritional stimuli [17].
Recent evidence has also linked age-related obesity to the pathogenesis of sarcopenia. As adipose tissue redistributes to the visceral area and infiltrates into muscle with age, it results in local myosteatosis, inducing mitochondrial dysfunction, reduction in β-oxidation of fatty acids, and production of reactive oxygen species [18]. This triggers low-grade chronic inflammation and systemic insulin resistance via proinflammatory cytokines and chemokines, resulting in the suppression of protein synthesis, stimulation of protein catabolism, and muscle atrophy [19]. Overall, these mechanisms cause an impaired balance between protein synthesis and proteolysis, yielding sarcopenia.
Extrinsic factors include lifestyle factors such as prolonged bed rest, surgical stress, malnutrition, or chronic disease. These processes are further intensified in the perioperative period, when patients undergoing gastrointestinal surgery typically fasted and sedentary for prolonged recovery periods, decelerating perioperative protein synthesis. Surgery also provokes a proinflammatory response that exacerbates muscle atrophy. It is therefore imperative to combat preoperative sarcopenia, which affects a myriad of adverse postoperative outcomes.
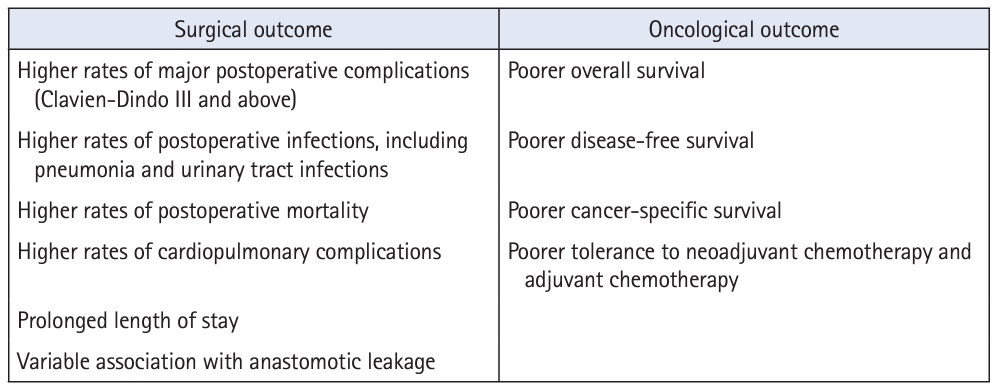
A summary of the impacts of sarcopenia on surgical and oncological outcomes is detailed in Fig. 2.
Sarcopenia is an independent predictor of poor surgical outcomes. It is associated with higher postoperative mortality in emergency general surgery [20–24], abdominal trauma [25], gastric cancer [26], hepatocellular carcinoma [27], pancreatic cancer [28], and biliary cancer [29]—and colorectal cancer is no exception. A meta-analysis of 44 observational studies comprising 18,891 patients with colorectal cancer conducted by Trejo-Avila et al. [30] revealed an association between sarcopenia and a higher risk of total postoperative complications, including infections and cardiopulmonary complications. Sarcopenia was also found to be significantly correlated with general postoperative infections at locations other than surgical sites, such as pneumonia and urinary tract infections [31]. A possible mechanism for occurrence is that sarcopenia causes an increased postoperative inflammatory response, as evidenced by significantly higher plasma concentrations of inflammatory markers such as calprotectin [32] and the neutrophil to lymphocyte ratio [33]. Amongst all postoperative complications, most studies on anastomotic leakage showed no significant difference in occurrence according to the presence or absence of sarcopenia [30, 31] except for 1 study [34] that found psoas density to be an independent predictor for anastomotic leakage. The heterogeneity of outcomes in the literature is largely attributable to variations in the definitions of sarcopenia used by publications and the type of measurements they have utilized, highlighting that standardized diagnostic methods should be adopted.
Sarcopenia has been associated with incomplete neoadjuvant treatment and poor tolerance to postoperative chemotherapy, with resultant effects on prognosis and overall survival [35]. Reduced muscle mass renders patients more susceptible to toxic effects during chemotherapy and thereby reduces treatment efficacy, possibly attributable to alterations in the pharmacokinetics of the drugs [36].
Several meta-analyses have also demonstrated that patients with sarcopenia have significantly shorter overall survival, disease-free survival, and cancer-specific survival than patients without sarcopenia [7, 30]. These results emphasize the crucial role of the early detection and prevention of sarcopenia in patients with colorectal cancer.
The mechanisms underlying unfavorable oncological outcomes in patients with sarcopenia are poorly understood. One hypothesis hints at an immunological impact associated with poor muscle health. Skeletal muscle has been shown to be associated with tumor‐infiltrating lymphocytes (TILs) in patients with colorectal cancer, where increased TILs (e.g., CD3+, CD8+, CD4+, and FOXP3+ T cells) may not only provide strong host immune reactions against cancer cell proliferation [37] but also effectively predict response to chemotherapy [38]. This mechanism is not unique to colorectal cancer, and these clinical findings have been replicated in gastric cancer, gynecological malignancies, and hepatobiliary cancers.
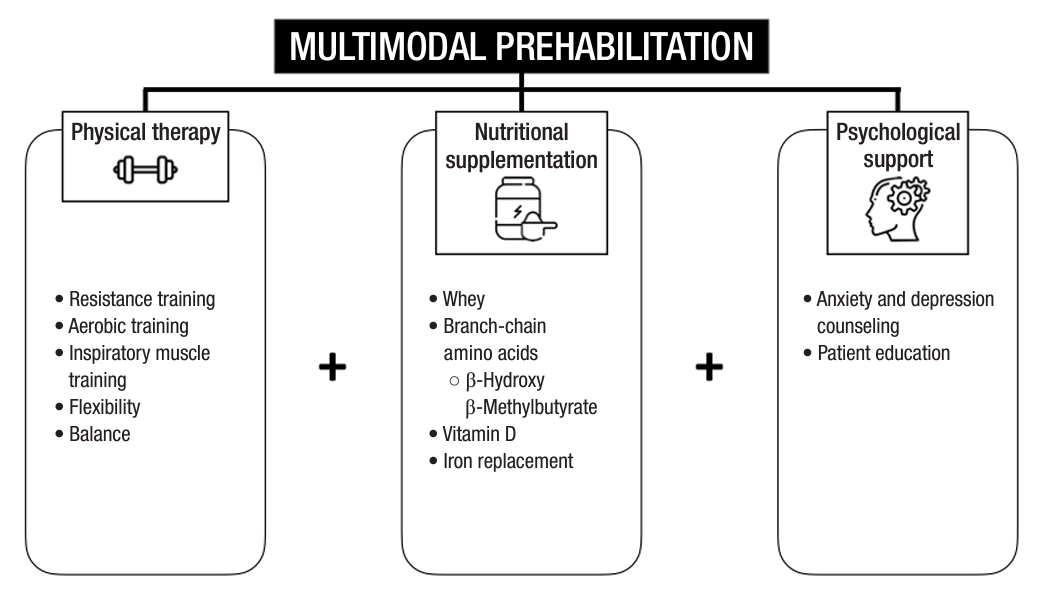
The concept of prehabilitation is based on the notion that the presurgical period is a “window of opportunity” to boost and optimize the premorbid nutrition of a patient, providing a compensatory “buffer” of physiological reserve for the impending insult of a surgical procedure [39]. This can be achieved through a multimodal prehabilitation program comprising nutrition, exercise, patient education, a comprehensive geriatric assessment, and quality of life assessments to improve patients’ physical fitness and capacity, optimize nutritional status, and promote psychological resilience (Fig. 3). Careful patient screening and selection to identify sarcopenic individuals preoperatively and address risk factors of poor muscle health with multimodal interventions can reduce potential perioperative adverse outcomes. A structured prehabilitation program especially for the geriatric population has been shown to shorten hospitalization, improve the rate of return to bowel activity, reduce the costs of hospitalization, and improve quality of life after surgery [40–43].
Exercise and physical therapy have been demonstrated to improve physical fitness, enhance quality of life, alleviate psychological anxiety and depression, and reduce fatigue during cancer treatment [44], and have been the mainstay of unimodal prehabilitation programs for colorectal cancer patients. Exercise modalities include aerobic training, resistance training, flexibility, and balance.
Resistance training, in particular, is known to promote muscle hypertrophy and increase muscle mass, strength, and function [45], and can be widely adopted even in frail elderly patients. These measures have objectively showed improvements in peak oxygen uptake [46], daily step count [47], and 6-minute walking test scores [48], which have translatable effects on the length of stay, readmission rates, tolerance to neoadjuvant treatment, and postoperative outcomes [44]. Exercise interventions also have impacts beyond physical fitness, showing improvements in depression and anxiety symptoms and quality of life scores [49].
Preoperative nutritional supplementation for at-risk individuals can increase preoperative muscle mass and strength. The potential for postoperative oral nutrition for postdischarge patients after colorectal cancer surgery in reducing sarcopenia prevalence has also been demonstrated in a randomized controlled trial showing a higher skeletal muscle index in patients who received oral nutritional supplementation than in those who received dietary advice alone [50].
The optimal type and regimen for oral supplementation for sarcopenia and the improvement of muscle strength remain unknown, possibly due to the fact that nutritional supplementation should not be a “one-size-fit-all” strategy, but rather one that is personalized and tailored to the metabolic needs and demands of different patients. Nevertheless, various schools of thought exist regarding the type of nutritional supplementation required for perioperative patients. For muscle synthesis and anabolism, protein supplementation has been the mainstay of nutritional prehabilitation in many studies. One common form of protein is whey protein, which is extracted from cow’s milk, containing all 9 essential amino acids required for anabolic processes. Whey protein also contains high amounts of cysteine, which contributes to the synthesis of intracellular glutathione, a dietary oxidant that has been shown to reduce oxidative stress in sarcopenic patients, especially under surgical stress [51]. Other studies have evaluated the effect of branched-chain amino acids, constituting leucine, isoleucine, and valine, which have shown positive impacts on muscle mass and strength [52]. β-Hydroxy-β-methylbutyrate (HMB), an active metabolite of leucine, which has well-established impacts on muscle strength in the elderly population [53], is being evaluated for similar efficacy in the preoperative prehabilitative setting. An ongoing study in Singapore, in partnership with Abbott Nutrition—the HEROS (Oral Nutritional Supplementation With HMB Enhance Muscle Quality in Sarcopenic Surgical Patients) study—has set out to evaluate the effects of HMB supplementation on intramuscular adipose tissue in the setting of multimodal prehabilitation for major gastrointestinal surgery patients [54].
Other nutrients also play a role in supplementing the anabolic response, and vitamin D is widely known to have benefits for muscle contraction, energy metabolism, and function via its effects on protein synthesis, skeletal muscle hypertrophy, and regulation of mitochondrial oxidative phosphorylation [55]. Preoperative intravenous iron supplementation and correction of iron deficiency anemia have been found to significantly reduce postoperative complications and the need for postoperative transfusions, which negatively impact disease-free survival [56].
It is expected that patients who have been diagnosed with colorectal cancer face a significant amount of stress, depression, and anxiety, which have direct effects on poorer surgical outcomes, including heightened pain sensitivity [57] and impaired wound healing from glucocorticoid production. The prevalence of depression and anxiety among colorectal cancer patients is as high as 57% and 47%, respectively [58], emphasizing the importance of early identification and treatment. Patients can be screened using validated questionnaires, such as the Generalized Anxiety Disorder-7 (GAD-7) and Patient Health Questionnaire-9 (PHQ-9). Several studies have attempted to provide psychological support in the form of breathing and relaxation exercises, as well as cognitive behavioral therapy.
The synergistic effects of nutritional therapy, physical exercise and psychological support have been well demonstrated; not only do dietary and physical activity interventions have positive effects on quality of life [59], but an improved outlook on life also affects compliance with treatment and therapeutics, thus underscoring the importance of a multimodal approach.
Compliance is an important element of prehabilitation. For use in practice, the tools employed need to be cost-effective, standardized, and repeatable by practitioners in a variety of clinical settings and across different patient populations. Targeting patients at risk, combining protein supplements with strength training, and defining standardized patient-related outcomes will be essential for obtaining satisfactory results [60].
Sustained treatment for sarcopenia seems to confer benefits even postoperatively, as seen in a retrospective cohort study by Lee et al. [61] involving 2,333 patients, where both overall survival and recurrence-free survival were lower in patients with persistent sarcopenia 2 to 3 years postoperatively than in those who recovered (overall survival: 96.2% vs. 90.2%, P=0.001; recurrence-free survival: 91.1% vs. 83.9%, P=0.002).
The indiscriminate inclusion of patients with colorectal cancer in prehabilitation programs may incur excessive healthcare costs and utilization of resources. In order to maximize benefits from a curated multidisciplinary prehabilitation program, resources should be targeted at patient groups who require it the most, such as those with sarcopenia and frailty. To date, no study has conclusively demonstrated the cost-effectiveness of such initiatives.
High-risk individuals who are elderly, frail, or manifest risk factors for sarcopenia, such as the presence of chronic conditions (heart failure, chronic obstructive pulmonary disease, diabetes mellitus, chronic kidney disease), functional decline, unintentional weight loss, repeated falls, and malnutrition [62], should be selected for objective measurements of sarcopenia based on muscle strength, physical performance, or skeletal muscle mass. While screening tools such as the SARC-F (Strength, Assistance walking, Rising from a chair, Climbing stairs, and Falls) questionnaire [63] exist for sarcopenia in the elderly, these tools have low sensitivity and have yet to be validated against CT-diagnosed sarcopenia [64]. CT-defined sarcopenia and myosteatosis are prevalent in preoperative colorectal cancer patients regardless of the presence of traditional nutritional risk factors (weight loss and problems eating); therefore, CT image analysis effectively adds value to nutrition screening by identifying patients with other risk factors for poor outcomes [65].
At the authors’ institution, a philanthropically sponsored prehabilitation program was initiated for patients 70 years old and above scheduled to undergo major colectomies [40]. These interventions included the following: (1) 3 weeks of oral nutrition supplementation recommended by the dietetics team; (2) 3 weeks of resistance exercises using resistance bands with weekly physiotherapist review; (3) a geriatrician consultation to optimize polypharmacy and other comorbidities among the “geriatric giants”; and (4) a thorough cardiovascular consult including preoperative transthoracic echocardiography to optimize preoperative cardiac risk. A comparison with patients with similar baseline characteristics who did not undergo the program showed a significantly shorter length of hospitalization, improvement in quality of life (based on the EuroQol-5 dimension score), and reduced costs, although anthropometric and functional characteristics, as well as morbidity rates, remained similar. The relatively short duration of the intervention could be a plausible explanation accounting for the absence of observed differences regarding measurable physical and functional attributes prior to surgery, which have been observed in the other studies mentioned above.
Present studies on prehabilitation in colorectal surgery are very heterogeneous in terms of the interventions and measured outcomes, hindering the standardization and adoption of this approach in clinical practice [44]. There are currently no standardized multimodal prehabilitation programs available, although efforts are being made to design and test formulated interventions through ongoing randomized controlled trials [66, 67]. A multimodal program inevitably requires an orchestrated effort and mobilization of resources from various disciplines, including physicians, surgeons, therapists, and nutritionists, and the cost-effectiveness of such an approach will need to be further evaluated.
Another major limitation is that the currently available studies on prehabilitation have mostly recruited patients using a “one-size-fits-all” approach, which may skew the results to show little or no significant effect. A selective approach to targeting only high-risk patients, who will reap more benefits from such programs, may allow us to observe better outcomes.
While current treatment strategies for sarcopenia focus on lifestyle modification and nutritional supplementation, these therapies have limited benefit to those who are immobile or unable to tolerate preoperative enteral nutrition. Novel therapeutics through the identification of targetable regions for cellular interventions are being evaluated as potential future treatments of sarcopenia. Multiomics profiling studies have been conducted to establish a comprehensive understanding of molecular changes and signaling networks involved in the pathogenesis of sarcopenia, which may lead to new clinical applications [68]. The use of regenerative medicine and stem cell therapy, which have mitochondrial restoration effects and immune modulatory abilities, offers potential for new promising therapies that may enable sarcopenia treatment on a molecular level [69].
At the same time, new modalities of assessing sarcopenia have been under development, with devices utilizing point-of-care ultrasound technology to measure intramuscular adipose tissue as a rapid assessment tool [70]. This potentially enables interval assessments of sarcopenia to track patients’ functional changes at regular intervals to monitor the efficacy of the prehabilitation program.
It is foreseeable that a multimodal, multidisciplinary approach modulated to suit an individual’s unique clinical, lifestyle, and molecular profile can be employed to combat this increasing health problem in our aging population.
Sarcopenia is prevalent in the aging population and negatively impacts surgical and oncological outcomes, as well as quality of life. Multimodal prehabilitation might be the way forward for improving outcomes, with promising data in selected groups of patients. Deeper scientific studies with close translation to clinical practice coupled with industrial collaboration can further refine the management of sarcopenia.
Notes
REFERENCES
1. Petermann-Rocha F, Balntzi V, Gray SR, Lara J, Ho FK, Pell JP, et al. Global prevalence of sarcopenia and severe sarcopenia: a systematic review and meta-analysis. J Cachexia Sarcopenia Muscle 2022;13:86–99.




2. Gillis C, Ljungqvist O, Carli F. Corrigendum to 'Prehabilitation, enhanced recovery after surgery, or both? A narrative review' (Br J Anaesth 2022; 128: 434-48). Br J Anaesth 2022;128:1061.


3. Fielding RA, Vellas B, Evans WJ, Bhasin S, Morley JE, Newman AB, et al. Sarcopenia: an undiagnosed condition in older adults: current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc 2011;12:249–56.



4. Studenski SA, Peters KW, Alley DE, Cawthon PM, McLean RR, Harris TB, et al. The FNIH sarcopenia project: rationale, study description, conference recommendations, and final estimates. J Gerontol A Biol Sci Med Sci 2014;69:547–58.



5. Chen LK, Woo J, Assantachai P, Auyeung TW, Chou MY, Iijima K, et al. Asian Working Group for Sarcopenia: 2019 consensus update on sarcopenia diagnosis and treatment. J Am Med Dir Assoc 2020;21:300–7.


6. Cruz-Jentoft AJ, Bahat G, Bauer J, Boirie Y, Bruyère O, Cederholm T, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 2019;48:601.




7. Xie H, Wei L, Liu M, Yuan G, Tang S, Gan J. Preoperative computed tomography-assessed sarcopenia as a predictor of complications and long-term prognosis in patients with colorectal cancer: a systematic review and meta-analysis. Langenbecks Arch Surg 2021;406:1775–88.



8. Derstine BA, Holcombe SA, Goulson RL, Ross BE, Wang NC, Sullivan JA, et al. Quantifying sarcopenia reference values using lumbar and thoracic muscle areas in a healthy population. J Nutr Health Aging 2017;21:180–5.


9. Nijholt W, Scafoglieri A, Jager-Wittenaar H, Hobbelen JS, van der Schans CP. The reliability and validity of ultrasound to quantify muscles in older adults: a systematic review. J Cachexia Sarcopenia Muscle 2017;8:702–12.




10. Sinelnikov A, Qu C, Fetzer DT, Pelletier JS, Dunn MA, Tsung A, et al. Measurement of skeletal muscle area: comparison of CT and MR imaging. Eur J Radiol 2016;85:1716–21.


11. Shafiee G, Keshtkar A, Soltani A, Ahadi Z, Larijani B, Heshmat R. Prevalence of sarcopenia in the world: a systematic review and meta-analysis of general population studies. J Diabetes Metab Disord 2017;16:21.




12. Martone AM, Bianchi L, Abete P, Bellelli G, Bo M, Cherubini A, et al. The incidence of sarcopenia among hospitalized older patients: results from the Glisten study. J Cachexia Sarcopenia Muscle 2017;8:907–14.




13. Shen Y, Chen J, Chen X, Hou L, Lin X, Yang M. Prevalence and associated factors of sarcopenia in nursing home residents: a systematic review and meta-analysis. J Am Med Dir Assoc 2019;20:5–13.


14. Pamoukdjian F, Bouillet T, Lévy V, Soussan M, Zelek L, Paillaud E. Prevalence and predictive value of pre-therapeutic sarcopenia in cancer patients: a systematic review. Clin Nutr 2018;37:1101–13.


15. Bossi P, Delrio P, Mascheroni A, Zanetti M. The spectrum of malnutrition/cachexia/sarcopenia in oncology according to different cancer types and settings: a narrative review. Nutrients 2021;13:1980.



16. Huang DD, Wang SL, Zhuang CL, Zheng BS, Lu JX, Chen FF, et al. Sarcopenia, as defined by low muscle mass, strength and physical performance, predicts complications after surgery for colorectal cancer. Colorectal Dis 2015;17:O256–64.


17. Paddon-Jones D, Rasmussen BB. Dietary protein recommendations and the prevention of sarcopenia. Curr Opin Clin Nutr Metab Care 2009;12:86–90.



18. Li CW, Yu K, Shyh-Chang N, Jiang Z, Liu T, Ma S, et al. Pathogenesis of sarcopenia and the relationship with fat mass: descriptive review. J Cachexia Sarcopenia Muscle 2022;13:781–94.




19. Bano G, Trevisan C, Carraro S, Solmi M, Luchini C, Stubbs B, et al. Inflammation and sarcopenia: a systematic review and meta-analysis. Maturitas 2017;96:10–5.


20. Francomacaro LM, Walker C, Jaap K, Dove J, Hunsinger M, Widom K, et al. Sarcopenia predicts poor outcomes in urgent exploratory laparotomy. Am J Surg 2018;216:1107–13.


21. McQuade C, Kavanagh DO, O'Brien C, Hunter K, Nally D, Hickie C, et al. CT-determined sarcopenia as a predictor of post-operative outcomes in patients undergoing an emergency laparotomy. Clin Imaging 2021;79:273–7.


22. Trotter J, Johnston J, Ng A, Gatt M, MacFie J, McNaught C. Is sarcopenia a useful predictor of outcome in patients after emergency laparotomy? A study using the NELA database. Ann R Coll Surg Engl 2018;100:377–81.



23. Du Y, Karvellas CJ, Baracos V, Williams DC, Khadaroo RG; Acute Care and Emergency Surgery (ACES) Group. Sarcopenia is a predictor of outcomes in very elderly patients undergoing emergency surgery. Surgery 2014;156:521–7.


24. Ming YJ, Howley P, Holmes M, Gani J, Pockney P. Sarcopenia 'made simple' and outcomes from emergency laparotomy. ANZ J Surg 2022;92:3198–203.




25. Kaplan SJ, Zhao KL, Koren M, Bentov I, Reed MJ, Pham TN. Thresholds and mortality associations of paraspinous muscle sarcopenia in older trauma patients. JAMA Surg 2020;155:662–4.



26. Huang DD, Chen XX, Chen XY, Wang SL, Shen X, Chen XL, et al. Sarcopenia predicts 1-year mortality in elderly patients undergoing curative gastrectomy for gastric cancer: a prospective study. J Cancer Res Clin Oncol 2016;142:2347–56.



27. Voron T, Tselikas L, Pietrasz D, Pigneur F, Laurent A, Compagnon P, et al. Sarcopenia impacts on short- and long-term results of hepatectomy for hepatocellular carcinoma. Ann Surg 2015;261:1173–83.


28. Peng P, Hyder O, Firoozmand A, Kneuertz P, Schulick RD, Huang D, et al. Impact of sarcopenia on outcomes following resection of pancreatic adenocarcinoma. J Gastrointest Surg 2012;16:1478–86.




29. Chakedis J, Spolverato G, Beal EW, Woelfel I, Bagante F, Merath K, et al. Pre-operative sarcopenia identifies patients at risk for poor survival after resection of biliary tract cancers. J Gastrointest Surg 2018;22:1697–708.



30. Trejo-Avila M, Bozada-Gutiérrez K, Valenzuela-Salazar C, Herrera-Esquivel J, Moreno-Portillo M. Sarcopenia predicts worse postoperative outcomes and decreased survival rates in patients with colorectal cancer: a systematic review and meta-analysis. Int J Colorectal Dis 2021;36:1077–96.



31. Nakanishi R, Oki E, Sasaki S, Hirose K, Jogo T, Edahiro K, et al. Sarcopenia is an independent predictor of complications after colorectal cancer surgery. Surg Today 2018;48:151–7.



32. Reisinger KW, Derikx JP, van Vugt JL, Von Meyenfeldt MF, Hulsewé KW, Olde Damink SW, et al. Sarcopenia is associated with an increased inflammatory response to surgery in colorectal cancer. Clin Nutr 2016;35:924–7.


33. Abbass T, Dolan R, McSorley ST, Horgan PG, McMillan DC. Association of sarcopenia and myosteatosis with the systemic inflammatory response and tumor stage in patients undergoing surgery for colorectal cancer (CRC). J Clin Oncol 2020;38(4_suppl):130.

34. Herrod PJ, Boyd-Carson H, Doleman B, Trotter J, Schlichtemeier S, Sathanapally G, et al. Quick and simple; psoas density measurement is an independent predictor of anastomotic leak and other complications after colorectal resection. Tech Coloproctol 2019;23:129–34.




35. Abe S, Nozawa H, Kawai K, Sasaki K, Murono K, Emoto S, et al. Poor nutrition and sarcopenia are related to systemic inflammatory response in patients with rectal cancer undergoing preoperative chemoradiotherapy. Int J Colorectal Dis 2022;37:189–200.



36. Antoun S, Borget I, Lanoy E. Impact of sarcopenia on the prognosis and treatment toxicities in patients diagnosed with cancer. Curr Opin Support Palliat Care 2013;7:383–9.


37. Daitoku N, Miyamoto Y, Hiyoshi Y, Tokunaga R, Sakamoto Y, Sawayama H, et al. Preoperative skeletal muscle status is associated with tumor-infiltrating lymphocytes and prognosis in patients with colorectal cancer. Ann Gastroenterol Surg 2022;6:658–66.




38. Mlecnik B, Bifulco C, Bindea G, Marliot F, Lugli A, Lee JJ, et al. Multicenter international Society for Immunotherapy of Cancer study of the consensus immunoscore for the prediction of survival and response to chemotherapy in stage III colon cancer. J Clin Oncol 2020;38:3638–51.



39. Koh FH, Chua JM, Tan JL, Foo FJ, Tan WJ, Sivarajah SS, et al. Paradigm shift in gastrointestinal surgery: combating sarcopenia with prehabilitation: multimodal review of clinical and scientific data. World J Gastrointest Surg 2021;13:734–55.



40. Koh FH, Loh CH, Tan WJ, Ho LM, Yen D, Chua JM, et al. Structured presurgery prehabilitation for aged patients undergoing elective surgery significantly improves surgical outcomes and reduces cost: a nonrandomized sequential comparative prospective cohort study. Nutr Clin Pract 2022;37:645–53.




41. Jain SR, Kandarpa VL, Yaow CY, Tan WJ, Ho LM, Sivarajah SS, et al. The role and effect of multimodal prehabilitation before major abdominal surgery: a systemic review and meta-analysis. World J Surg 2023;47:86–102.


42. Gillis C, Buhler K, Bresee L, Carli F, Gramlich L, Culos-Reed N, et al. Effects of nutritional prehabilitation, with and without exercise, on outcomes of patients who undergo colorectal surgery: a systematic review and meta-analysis. Gastroenterology 2018;155:391–410.e4.


43. Molenaar CJ, van Rooijen SJ, Fokkenrood HJ, Roumen RM, Janssen L, Slooter GD. Prehabilitation versus no prehabilitation to improve functional capacity, reduce postoperative complications and improve quality of life in colorectal cancer surgery. Cochrane Database Syst Rev 2022;5:CD013259.



44. Bausys A, Kryzauskas M, Abeciunas V, Degutyte AE, Bausys R, Strupas K, et al. Prehabilitation in modern colorectal cancer surgery: a comprehensive review. Cancers (Basel) 2022;14:5017.



45. Lichtenberg T, von Stengel S, Sieber C, Kemmler W. The favorable effects of a high-intensity resistance training on sarcopenia in older community-dwelling men with osteosarcopenia: the randomized controlled FrOST study. Clin Interv Aging 2019;14:2173–86.



46. Morielli AR, Usmani N, Boulé NG, Severin D, Tankel K, Joseph K, et al. Feasibility, safety, and preliminary efficacy of exercise during and after neoadjuvant rectal cancer treatment: a phase II randomized controlled trial. Clin Colorectal Cancer 2021;20:216–26.


47. Moug SJ, Barry SJ, Maguire S, Johns N, Dolan D, Steele RJ, et al. Does prehabilitation modify muscle mass in patients with rectal cancer undergoing neoadjuvant therapy? A subanalysis from the REx randomised controlled trial. Tech Coloproctol 2020;24:959–64.




48. de Klerk M, van Dalen DH, Nahar-van Venrooij LM, Meijerink WJ, Verdaasdonk EG. A multimodal prehabilitation program in high-risk patients undergoing elective resection for colorectal cancer: a retrospective cohort study. Eur J Surg Oncol 2021;47:2849–56.


49. Kraemer MB, Priolli DG, Reis IG, Pelosi AC, Garbuio AL, Messias LH. Home-based, supervised, and mixed exercise intervention on functional capacity and quality of life of colorectal cancer patients: a meta-analysis. Sci Rep 2022;12:2471.




50. Tan S, Meng Q, Jiang Y, Zhuang Q, Xi Q, Xu J, et al. Impact of oral nutritional supplements in post-discharge patients at nutritional risk following colorectal cancer surgery: a randomised clinical trial. Clin Nutr 2021;40:47–53.


51. Gilmartin S, O'Brien N, Giblin L. Whey for sarcopenia; can whey peptides, hydrolysates or proteins play a beneficial role? Foods 2020;9:750.



52. Kobayashi H. Amino acid nutrition in the prevention and treatment of sarcopenia. Yakugaku Zasshi 2018;138:1277–83. Japanese.


53. Courel-Ibáñez J, Vetrovsky T, Dadova K, Pallarés JG, Steffl M. Health benefits of β-hydroxy-β-methylbutyrate (HMB) supplementation in addition to physical exercise in older adults: a systematic review with meta-analysis. Nutrients 2019;11:2082.



54. Koh FH. Oral nutritional supplementation with HMB enhance muscle quality in sarcopenic surgical patients (HEROS). ClinicalTrials.gov identifier: NCT05344313 [Internet]. US National Library of Medicine; 2022 [cited 2022 Dec 20]. Available from: https://clinicaltrials.gov/ct2/show/NCT05344313
55. Uchitomi R, Oyabu M, Kamei Y. Vitamin D and sarcopenia: potential of vitamin D supplementation in sarcopenia prevention and treatment. Nutrients 2020;12:3189.



56. Kangaspunta M, Mäkijärvi J, Koskensalo S, Kokkola A, Arkkila P, Scheinin T, et al. Preoperative intravenous iron treatment reduces postoperative complications and postoperative anemia in preoperatively anemic patients with colon carcinoma. Int J Colorectal Dis 2022;37:449–55.




57. Tsimopoulou I, Pasquali S, Howard R, Desai A, Gourevitch D, Tolosa I, et al. Psychological prehabilitation before cancer surgery: a systematic review. Ann Surg Oncol 2015;22:4117–23.



58. Peng YN, Huang ML, Kao CH. Prevalence of depression and anxiety in colorectal cancer patients: a literature review. Int J Environ Res Public Health 2019;16:411.



59. Ho M, Ho JW, Fong DY, Lee CF, Macfarlane DJ, Cerin E, et al. Effects of dietary and physical activity interventions on generic and cancer-specific health-related quality of life, anxiety, and depression in colorectal cancer survivors: a randomized controlled trial. J Cancer Surviv 2020;14:424–33.




60. Bruns ER, Argillander TE, Van Den Heuvel B, Buskens CJ, Van Duijvendijk P, Winkels RM, et al. Oral nutrition as a form of pre-operative enhancement in patients undergoing surgery for colorectal cancer: a systematic review. Surg Infect (Larchmt) 2018;19:1–10.


61. Lee C, Park IJ, Kim KW, Shin Y, Lim SB, Kim CW, et al. Influence of postoperative changes in sarcopenia on long-term survival in non-metastatic colorectal cancer patients. Cancers (Basel) 2021;13:2410.



62. Gao Q, Hu K, Yan C, Zhao B, Mei F, Chen F, et al. Associated factors of sarcopenia in community-dwelling older adults: a systematic review and meta-analysis. Nutrients 2021;13:4291.



63. Nishikawa H, Asai A, Fukunishi S, Takeuchi T, Goto M, Ogura T, et al. Screening tools for sarcopenia. In Vivo 2021;35:3001–9.



64. Djordjevic A, Deftereos I, Carter VM, Morris S, Shannon R, Kiss N, et al. Ability of malnutrition screening and assessment tools to identify computed tomography defined low muscle mass in colorectal cancer surgery. Nutr Clin Pract 2022;37:666–76.



65. Klassen P, Baracos V, Gramlich L, Nelson G, Mazurak V, Martin L. Computed-tomography body composition analysis complements pre-operative nutrition screening in colorectal cancer patients on an enhanced recovery after surgery pathway. Nutrients 2020;12:3745.



66. van Rooijen S, Carli F, Dalton S, Thomas G, Bojesen R, Le Guen M, et al. Multimodal prehabilitation in colorectal cancer patients to improve functional capacity and reduce postoperative complications: the first international randomized controlled trial for multimodal prehabilitation. BMC Cancer 2019;19:98.



67. Amaro-Gahete FJ, Jurado J, Cisneros A, Corres P, Marmol-Perez A, Osuna-Prieto FJ, et al. Multidisciplinary prehabilitation and postoperative rehabilitation for avoiding complications in patients undergoing resection of colon cancer: rationale, design, and methodology of the ONCOFIT study. Nutrients 2022;14:4647.



68. Liu JC, Dong SS, Shen H, Yang DY, Chen BB, Ma XY, et al. Multi-omics research in sarcopenia: current progress and future prospects. Ageing Res Rev 2022;76:101576.