DISCUSSION
SLS has been shown to have multiple short-term patient benefits, including decreased postoperative pain, shorter hospital stay, earlier return of gastrointestinal function, faster return to normal activity, smaller incision, and fewer postoperative pulmonary and wound complications. On the other hand, the limitations of a purely laparoscopic approach include a relative lack of tactile feedback and the absence of depth perception; other limitations include the fact that SLS is a demanding technique with a steep learning curve and a longer operative time than open surgery, and the absence of gentle and safe laparoscopic retracting devices.
HALS allows the surgeon to place a nondominant hand within the abdominal cavity to assist in the use of laparoscopic instrumentation. A hand-assisted laparoscopic colectomy has been described as a hybrid procedure [
9] and was the first report of the HALS concept [
10]. Several advantages of the hand-assisted approach were emphasized: the inserted hand can provide blunt dissection, tactile feedback from the hand helps to identify lesions that are not clearly visible, and better control of bleeding and better organ retraction are possible. HALS, therefore, represents a useful alternative to SLS [
6,
11] and may be considered as a new method for more complex procedures or more difficult pathologies [
7,
12,
13]. However, the best use for HALS is laparoscopy-assisted surgery in which an additional incision is required for extracting the specimen. Therefore, HALS seems to be especially suited for colorectal surgery [
6,
7,
11].
Although HALS has been considered a means to help nonskilled surgeons through the long learning curve associated with performing a laparoscopic colectomy [
11,
14,
15], both HALS and SLS have made unique individual contributions to surgery. In this study, we view HALS as another tool in the surgeon's armamentarium that can be used in selected patients.
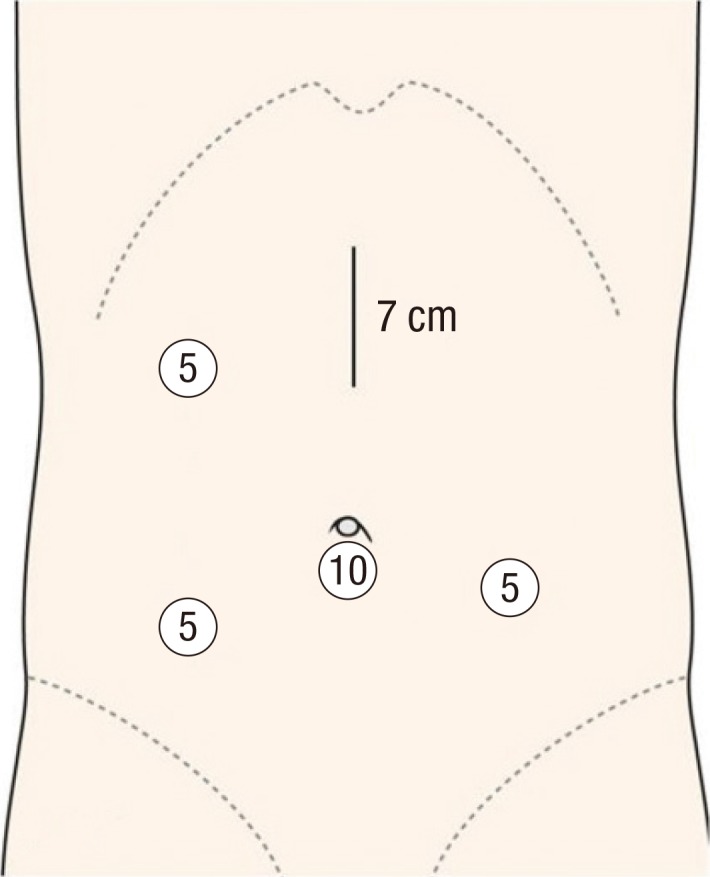
The location of the port placement is important because it can determine the range of blunt hand dissection whereas inappropriate port placement for the hand device may compromise the view of the camera. A trial [
8] of HALS and SLS for a laparoscopic RHC showed that patients who were this or had a short stature were better suited for SLS, as port placement for the hand device through the midline or Pfannenstiel incision might compromise the view of the camera. On the other hand, in the study of Schadde et al. [
16], the handport device was placed in the midline, and a 10-mm trocar was placed in the right upper quadrant for the camera, and Chung et al. [
17] suggested handport device placement through a lower abdominal midline incision. Ballantyne and Leahy [
18] preferred to place the handport device through an upper abdominal midline incision near the planned anastomosis, similar to the position of our handport device. The position of the port placement was determined by the location of the lesion, the location of anastomosis, and the side of the surgeon's dominant hand. If the surgeon can use both his or her nondominant hand and dominant hand in the abdominal cavity for HALS, in our opinion, this position of the handport placement is appropriate for a hand-assisted laparoscopic RHC.
In the current study, the surgeon inserted the handport device at the beginning of the procedure and then used it during the remainder of the operation. On the other hand, in the report of Chew and Adams [
19], the surgeon's left hand was placed through the Pfannenstiel incision, and the ascending colon, hepatic flexure, and proximal transverse colon were mobilized bluntly by using the left hand, which was then withdrawn from the handport device and replaced by diathermy scissors at the dissection of the lateral peritoneal attachments.
Several technical aspects are related to HALS. Lee et al. [
20] showed that a moist laparotomy pad could be inserted through the handport device and was used to gently pack the small intestine away from the pelvis. Nakajima et al. [
21] also described how surgical towels could be used to move the small intestine away from the operative site. Most handport devices could function as a wound protector, which should theoretically protect the HAL wound from tumor implantation. Recently, a modified laparoscopic technique was developed and is referred to as the HALS Finger-Mounted Instrument (Ethicon Endo-surgery Inc., Cincinnati, OH, USA), in which miniature forceps, graspers, scissors, dissectors, probes and retractors mounted on the surgeon's fingers can perform delicate surgical tasks.
In this study, 41 of 45 patients who underwent SLS underwent a RHC using a retroperitoneal approach. The retroperitoneal approach for a RHC is not popular and needs an additional 10-mm port. However, that approach, which takes about 15 minutes, is similar to the lateral or inferior approach in the sense that the dissection around the main vessels is performed after the dissection of retroperitoneal structures, such as the ureter, gonadal vessels, and the duodenum. The following are some advantages compared to the transabdominal approach:
Much of the retroperitoneal cavity can be created by only air insertion thorough the distension balloon.
An identification and dissection of the ureter and the gonadal vessels can be easily performed.
The surgical field is not disturbed by the small bowel.
The range of the dissection after the medial-to-lateral transabdominal approach can be decreased.
In our institute, this approach is commonly performed in a RHC except for (1) tumors larger than 6 cm and (2) tumors locally invading adjacent organs.
A previous prospective, randomized, multicenter study concluded that HALS had similar short-term clinical outcomes to SLS and resulted in significantly shorter operation times than SLS for patients who underwent a left-sided colectomy and a total abdominal colectomy [
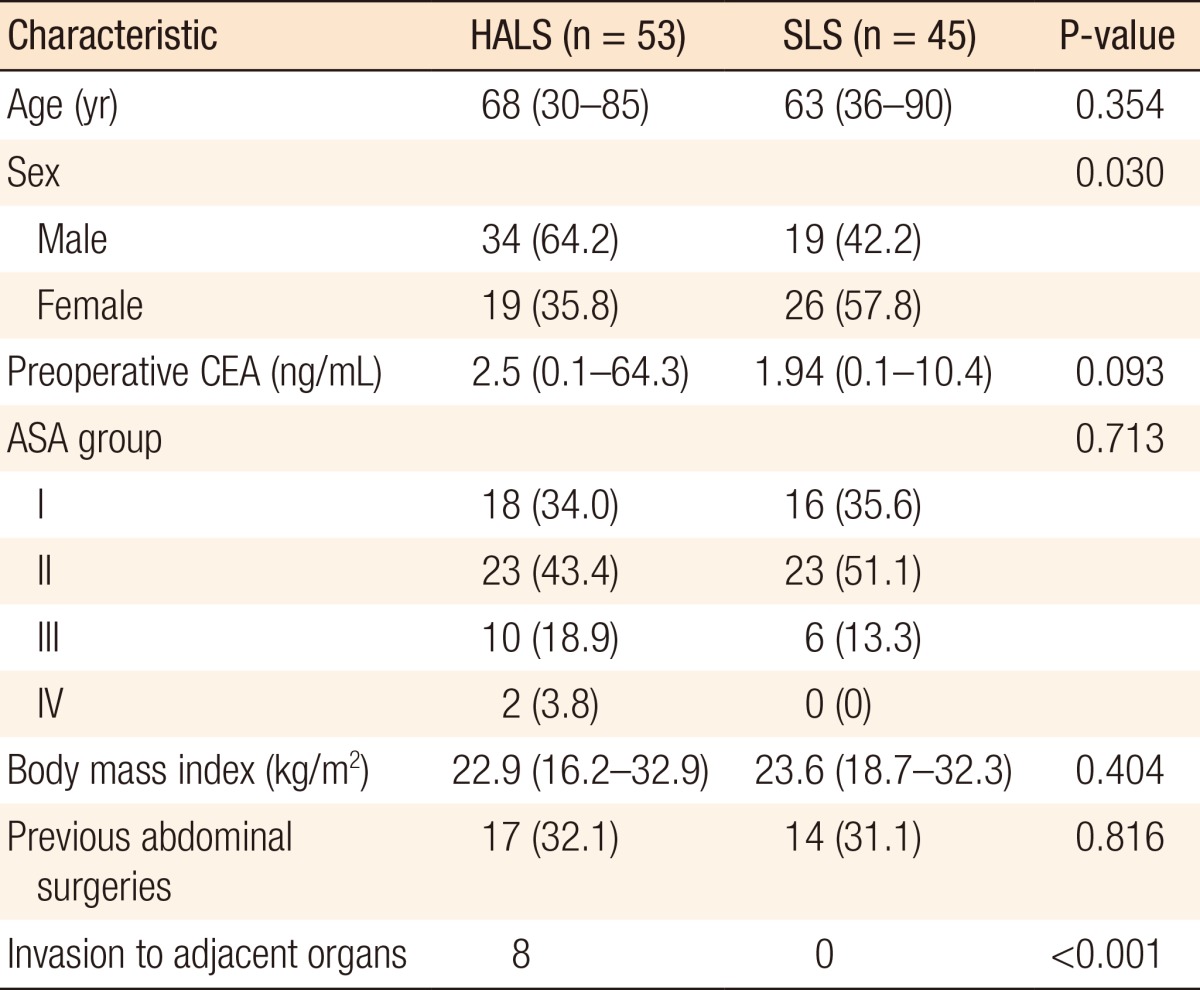
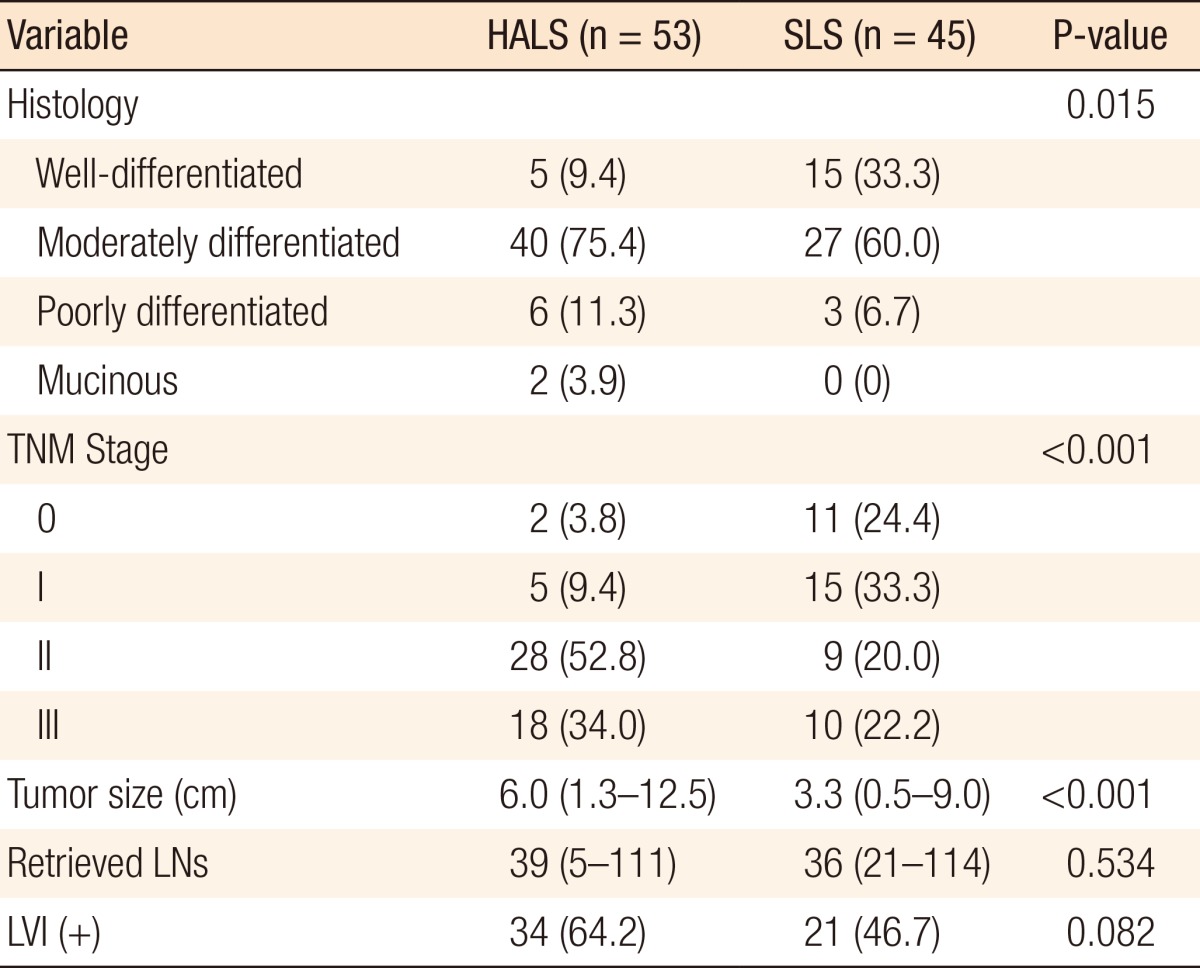
8]. In the present study, no significant difference in the median operation times were noted between the HALS and the SLS groups (318 minutes vs. 300 minutes, P = 0.330). The selection of patients for one approach versus the other was subject to significant selection biases, such as patient characteristics, disease and operative factors, and the surgeon's experience. The HALS resection group had a significantly higher pathologic TNM stage, which resulted in a significantly larger tumor size, than the SLS resection group. The patients in the HALS group were more likely than those in the SLS group to undergo concurrent resection of adjacent organs because of tumor invasion, reflecting the increased complexity of HALS procedures. Therefore, considering that more advanced tumors were prevalent in the HALS group compared with SLS group, the similar perioperative outcomes and long-term oncologic outcomes between the two groups of patients suggest that HALS is beneficial in selected patients.
Consistent with other studies showing that HALS allows surgeons to perform more extensive and complex procedures, such as a laparoscopic total colectomy or proctocolectomy [
22-
24], we found that use of HALS in a RHC for right-sided colon cancer allowed us to expand our minimally-invasive practice to patients who might not otherwise have been considered candidates for SLS while still retaining the perioperative patient-related benefits of minimally invasive surgery. Indications of HALS for colorectal diseases in our clinic are (1) cases in which tactile feedback is necessary, like hepatic metastasis and uncertain state of intestine, (2) cases in which force is necessary, like firm adhesion, invasion to adjacent organs, (3) difficult surgeries, like adhesive ileus and obstructing colon cancer, (4) time-consuming surgeries, like a total colectomy and a total proctocolectomy, (5) tumors larger than 6 cm, (6) surgeon's preference, HALS also being used as a routine procedure when the surgeon prefers that approach, and (7) patient with surgical and anesthetic high-risk to shorten the operation time.
The limitations of this study include its retrospective nature, the small size of the study, and the difference of pathologic TNM stage between the two groups. Therefore, a large, randomized, prospective study comparing short- and long-term outcomes between HALS and SLS for right-sided colon cancer is needed.
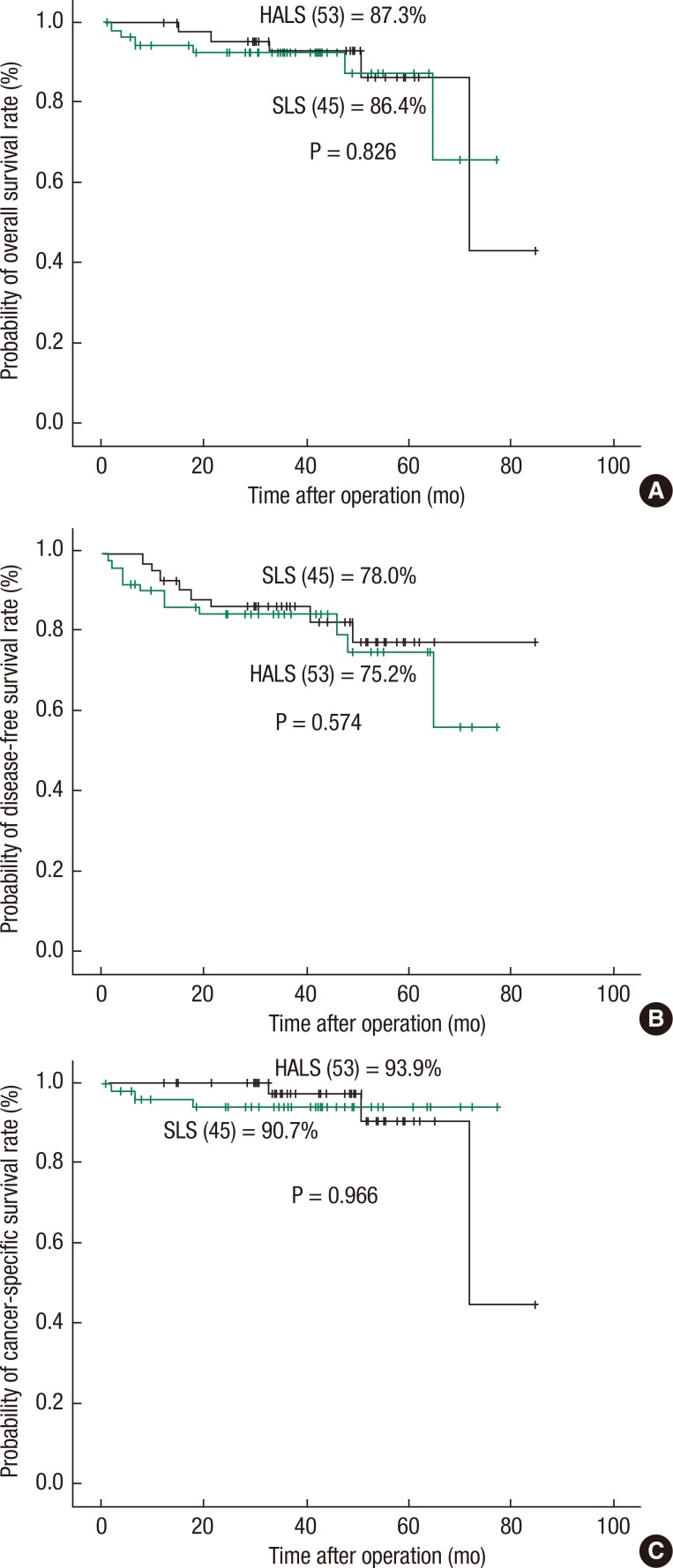
In conclusion, although patients in the HALS group had more advanced disease and underwent more complex procedures than those in the SLS group, the short-term benefits and the oncologic outcomes between the two groups were comparable. HALS can, therefore, be considered an alternative to SLS for bulky and fixed right-sided colon cancer.